How To Get The Best Result From Your Hip Or Knee Replacement Surgery
How To Get The Best Result From Your Hip Or Knee Replacement Surgery
By Allen Letgolts, Doctor of Physical Therapy
There are well-established protocol treatments for after joint replacement surgery, but many miss essential elements needed for full recovery. Despite a successful surgery,, many people still experience pain and lack mobility even many months later. They often blame the surgery, but the true cause is usually incomplete or inadequate rehabilitation.
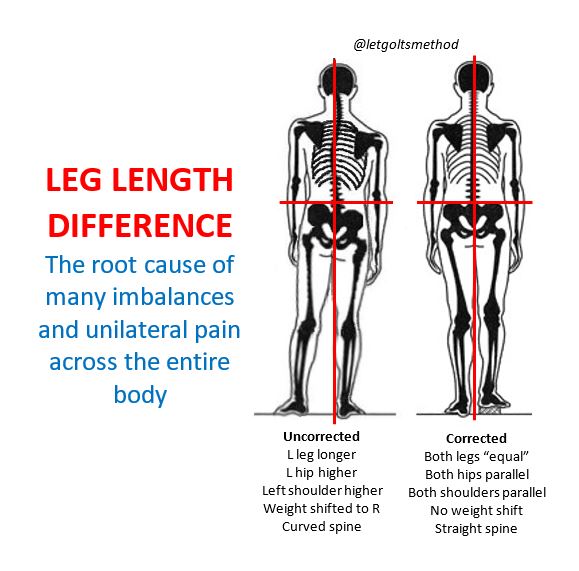
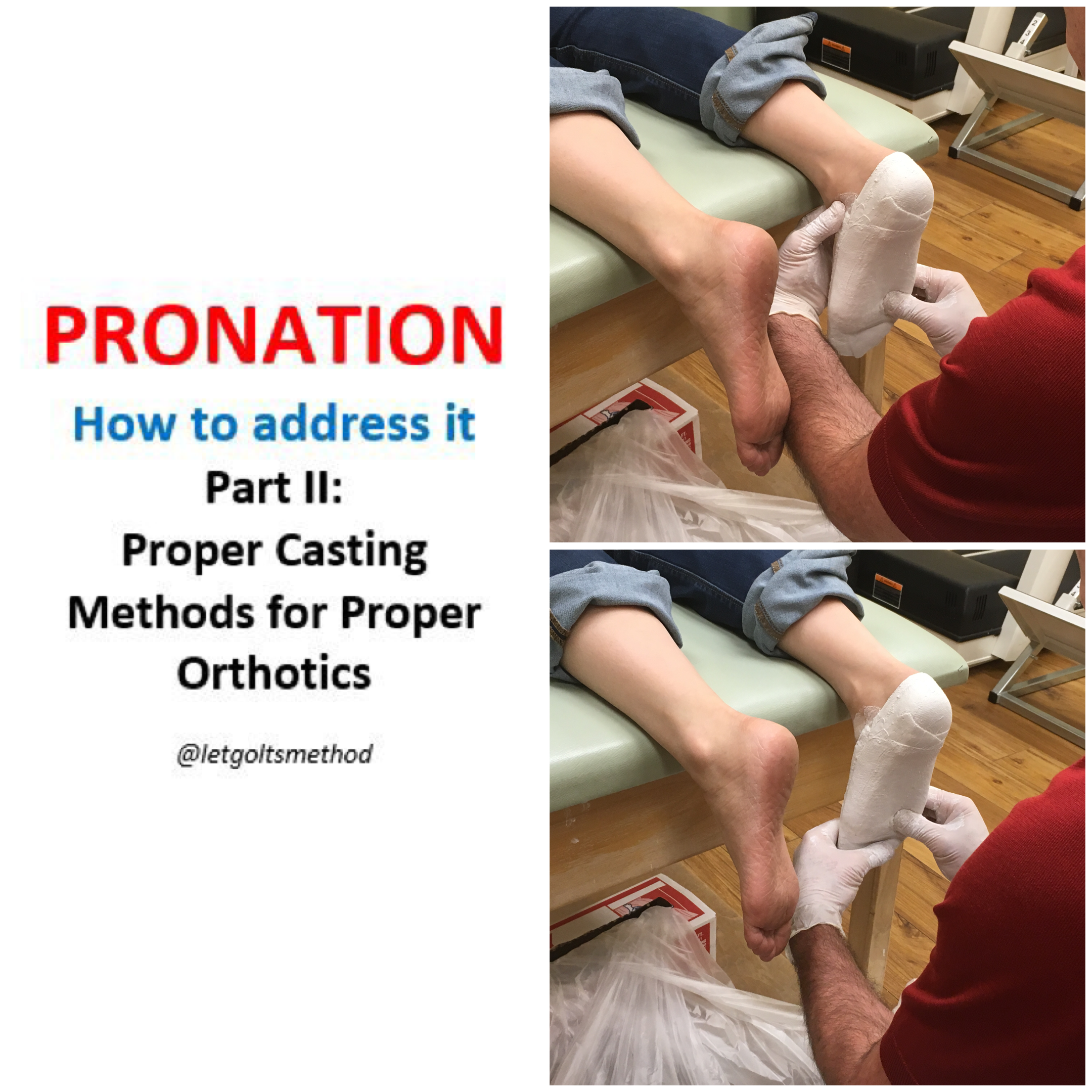
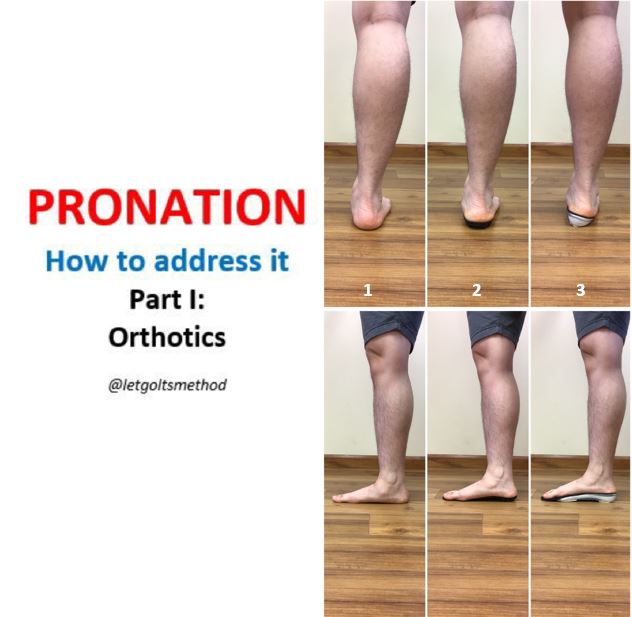
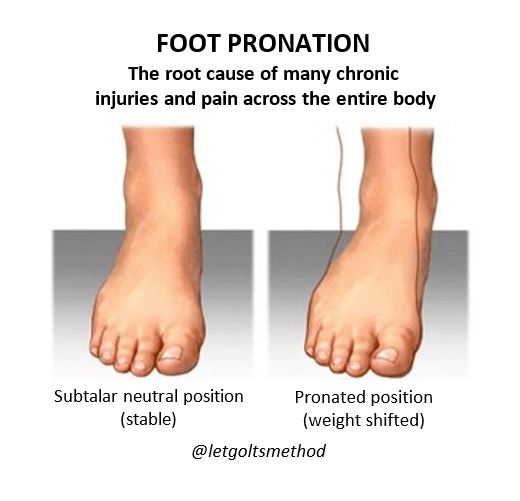
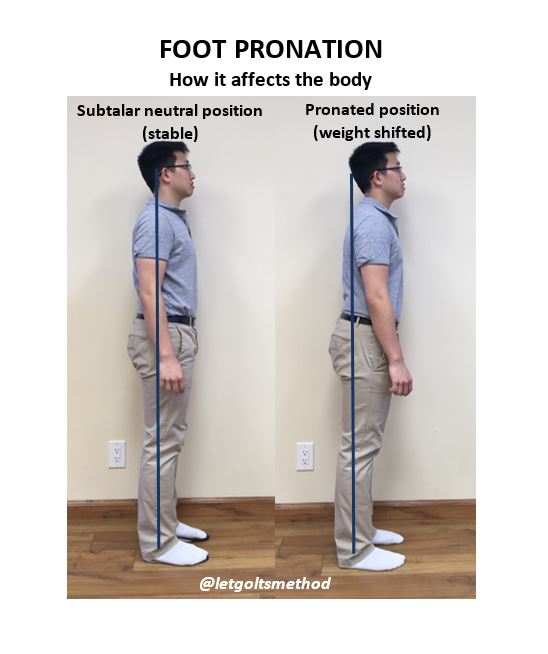
Most large joint damage happens over a long time, and is due to structural issues or prior injuries causing compensations. Of the many structural issues, the most common are pronation and a difference in people’s leg lengths. These cause uneven load on the joints. Over the years, that causes uneven wear, arthritis, and uneven muscle strength. Addressing these common underlying issues involves orthotics and/or heel lifts and re-alignment and retraining of muscles and joints. This is usually not part of post-surgical rehabilitation protocol.
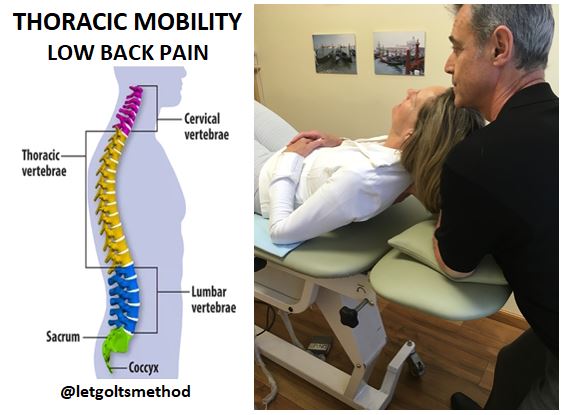
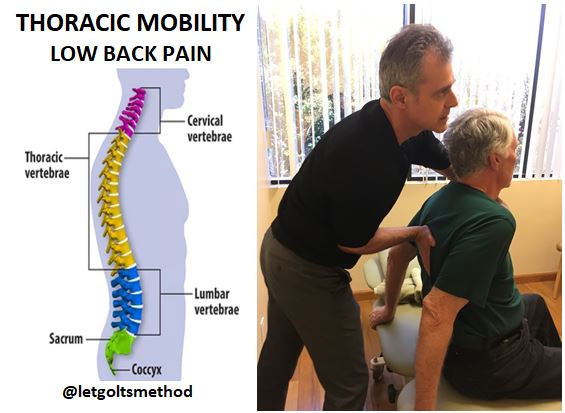
But prior injuries also impact joint health. An old sprained ankle that never healed properly. The twisted back that still flares up occasionally. These can cause improper knee movement, which can grind down the joint over time. Addressing a current or old injury involves manual manipulations to restore normal function of the joint.
It’s not only the underlying issues you have to address, if full recovery is your goal. It’s also the compensations that those issues caused. When a joint doesn’t function properly, itself is damaged, but due to damage it will also causes damage in other joints. When you have a structural issue or a prior injury, your body will automatically adapt and change the way it moves to avoid pain. Since this internal “passing the buck” simply shifts the uneven loading to elsewhere in your body, the trick is to identify the compensations, understand why and how they occur, and then address them.
Diagnosis of the cause of damage and resulting compensations is critical to post-surgical recovery. This is done by taking a careful history and doing a biomechanical analysis. The therapist should be able to explain clearly what the problem is and the proposed solution. Make sure to request that these issues be addressed in your post-surgical rehabilitation for best results.
Dr. Allen Letgolts DPT has been in private practice in Brentwood for over 20 years.
 Los Angeles Magazine’s Best Physical Therapy Practice in LA
Los Angeles Magazine’s Best Physical Therapy Practice in LA